To globally determine the physiological state of the organism, various parameters are determined: body temperature, arterial pulse (heart rate), blood pressure and respiratory rate. The measurement of these indicators serves to evaluate the activity of vital organs (brain, heart, lungs), their control being a basic nursing activity.
Nursing Considerations:
- Control and record vital signs at the time of admission of the person. These data, duly recorded in the nursing sheet, will be very useful as baseline values in subsequent clinical evaluations of the patient.
- The schedule established for the control of each center and the specific instructions for each case must always be strictly respected. Sometimes it is enough to carry out a daily measurement or in each nursing shift, but in other cases, in critical situations, it is essential to carry out a very frequent or practically constant control.
- It should always be investigated whether the person is familiar with the procedures to be practiced. It must be taken into account that a state of anxiety or fear can alter the results of the measurements, so the nature of the measurements must be explained to reassure the person.
Body temperature:
The internal temperature of the body remains practically constant above 37ºC, an essential requirement for metabolic processes to develop normally. However, even under normal conditions, the measurement results refer depending on the point where it is taken: the oral temperature is 36.5 – 37.2ºC, while the axillary temperature is somewhat lower (0.2 – 0′ 3ºC lower), and the rectal temperature is somewhat higher (0.3 – 0.4ºC higher).
Nursing Considerations
- Control of body temperature should be carried out periodically and at the intervals required for the particular clinical situation of each patient. If there are no precise indications, the basal temperature is recorded at least once in each shift; At night, if the measurement is not essential, the patient’s sleep tends to be respected.
- It is advisable to always take the temperature in the same place, choosing for each person an area where the measurements can be carried out repeatedly. For reasons of comfort and hygiene, it is usual to perform the determination in the axillary area, except when dealing with small children or when there are specific situations that require it (upper limb amputation, deep hypothermia…); In this case, the choice will be to measure oral or rectal temperature.
- You should never take the temperature in the mouth if you notice that the person cannot cooperate or there is a risk of the thermometer breaking. Measurement in the mouth is contraindicated in people with seizures, unconsciousness, disorientation and confusion, administration of oxygen by nasal tube, nasogastric catheterization and diseases of the mouth, nose or throat.
- In small children, it is advisable to take the rectal temperature and always at the end of the rest of the measurements, because the maneuvers can cause crying and thus alter the pulse and blood pressure.
- Once the thermometer is located, wait the corresponding time depending on the measurement area. Armpit minimum of 5 minutes. Mouth minimum of 3 minutes. Straight minimum of 3 minutes.
- After measurement, disinfect the thermometer.
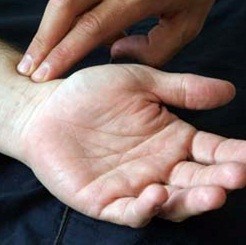
Arterial pulse:
The arterial pulse corresponds to the intermittent expansion that the arteries experience when the blood pumped by the heart circulates through them. It is produced from the propagation of impulses received by the wall of the aorta in each cardiac systole (heart rate). It is considered to be a good indicator of cardiac activity, because the pulse corresponds to the heartbeat. However, there are pathological circumstances that constitute an exception (arrhythmias) and require due comparison between the peripheral arterial pulse and the central pulse, determined by auscultation of cardiac activity with the stethoscope in the midclavicular line approximately in the fifth intercostal space. left. In adults, the most common place to take the pulse is the radial artery in the wrist. In babies, small children and unconscious people, it is usually taken in the carotid artery, in the neck or in the central pulse.
Nursing Considerations:
- Avoid taking the pulse with fingers that have their own pulse, such as the thumb and index finger, to avoid confusion; It is preferable to measure with the middle and ring fingers.
- It is not advisable to start counting immediately, but rather wait a few moments for the person to relax.
- Fingers should always be applied to the measurement area using very gentle initial pressure; if the pressure is strong. a weak pulse could go unnoticed.
- Count your pulses for a sufficient time, no less than 30 seconds, and if any irregularity is noted, for a minimum of 60 seconds.
- If there is a history of arrhythmia, the central pulse should be determined after the radial pulse.
- If the person has peripheral vascular pathology, it is advisable to record the pulse on both sides.
- Record the measurement specifying the frequency and other characteristics, as well as the point of measurement.
Blood pressure:
Blood pressure or tension (BP) corresponds to the force exerted by the blood driven by the heart on the arterial walls and that allows circulation throughout the arterial tree, overcoming peripheral resistance. Blood pressure is usually recorded in the arm (brachial artery), but if necessary (amputation, burns) it can be taken in the thigh (popliteal artery).
The measurement is carried out with the sphygmomanometer and a stethoscope; There are various types of sphygmomanometer (aneroid, electronic). The sphygmomanometer must have a cuff adapted to the patient’s characteristics, which corresponds to a width equivalent to two-thirds of the arm’s length, and a length sufficient to cover two-thirds of its circumference.
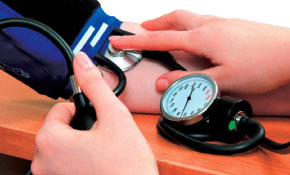
Technique:
- Explain the technique to the person.
- Place the person in a comfortable and relaxed position, with the arm extended and supported on a firm surface.
- Apply the cuff of the sphygmomanometer around the arm, leaving the elbow flexion area free.
- Locate the brachial pulse by palpation and place the membrane of the stethoscope in the area.
- Close the air valve and quickly inflate the cuff until the pulse disappears (180 mm Hg or more if the person is hypertensive, until the disappearance of the pulse is noted by palpation of the radial artery).
- Open the air valve and let the cuff deflate slowly, observing the pressure gauge scale and listening for the return of heartbeats with the stethoscope. The point at which the first noise is heard corresponds to the systolic or maximum pressure. The point at which the heartbeat stops being heard completely or there is a noticeable change in its clarity or intensity corresponds to the diastolic or minimum blood pressure.
- Completely deflate the cuff and remove the cuff.
- Record the measurement on the person’s chart, noting the systolic and diastolic pressure.
Nursing Considerations:
- If there is any doubt about the figures obtained, the procedure must be repeated.
- The measurement can be carried out with the person sitting or lying down, but making sure that the arm is located at the level of the heart.
- The presence of a state of anxiety or fear can alter the results.
Breathing frequency:
The determination consists of specifying the number of inspiration/expiration cycles that occur within one minute, observing the person’s chest to appreciate the depth of the movements. Furthermore, it is advisable to determine the characteristics of the respiratory movements, recording whether they are laborious, superficial, deep, etc. Under normal conditions, in an adult individual breathing has a frequency that ranges between 10 and 20 movements per minute, is regular and silent, and develops without any difficulty.
Nursing Considerations:
- If possible, ensure that the person does not notice the measurement, because any state of anxiety causes notable changes in respiratory rate.
- The measurement is carried out by simple observation of the thorax, but if the respiratory movements are barely perceptible, it is advisable to perform the determination by auscultation with the stethoscope in the right hemithorax for one minute.