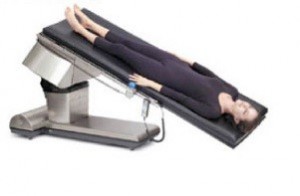
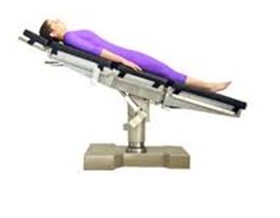
There are various characteristic positions that are used in various pathological situations or to carry out certain explorations and therapeutic or surgical practices.
When placing the person in a certain position, the following points should be checked:
1- That breathing is not hindered. It should not constrict the neck or chest.
2- That circulation is not hindered. If a restraint is made, the restraints should not be tight.
3- That no pressure or traction be exerted on any nerve. Sustained pressure on or stretching of peripheral nerves can cause sensory or motor loss.
4- That the pressure on the skin is reduced to a maximum, with a minimum of contact of the bone ridges on the support surface, to prevent pressure ulcers.
5- If an assistive or surgical procedure is to be carried out, there must be maximum accessibility to the site of action.
Whatever the person’s position, the alignment of the body must be monitored, ensuring that the different parts of the body maintain a correct relationship. In the person who is unconscious or with motor disorders, the limbs should be kept flexed in order to prevent muscle contractures.
The person’s response to the position in which they are placed should always be observed, modifying it as necessary to ensure the aforementioned points, either by regulating the planes of the bed or with the additional help of pillows or splints.
When a person spontaneously adopts an anti-pain posture, an attempt must be made to respect this position, unless it may cause or encourage complications.
Any disabled person who is bedridden for a long time should be changed position frequently, in order to prevent complications such as pressure ulcers. It is advisable to vary your position every 2-3 hours, during the 24 hours, following a specific guideline, for example: supine or Fowler’s position, left lateral decubitus, prone, right lateral decubitus, etc.
When an examination or care technique requires a position that is uncomfortable or embarrassing for the person, explain the need for it and ensure privacy through screens and curtains.
When a person’s position is modified with probes or tubing, care must be taken to ensure that they do not come out, obstruct or bend during the maneuver.
recumbent position
Decubitus is any position of the body in a state of rest on a horizontal plane. Depending on the part of the body in contact with the surface, different recumbent positions are differentiated.
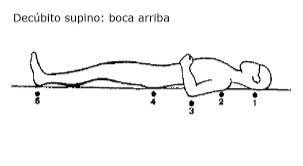
Supine or dorsal position
The person is lying face up, in a horizontal position, with the back in contact with the surface and the lower extremities extended.
Nursing Considerations:
It is the position that the person spontaneously tends to adopt in bed and the most used for explorations, maneuvers and surgical interventions on the anterior surface of the body, such as the abdominothoracic and some of the lower limbs.
It allows adequate lung expansion and facilitates the alignment of the different body segments.
When a disabled person has to remain supine for a long time, it is advisable to place a support on the feet, so that they remain supported and prevent them from falling (equinus pendulum foot). You should also avoid keeping your legs crossed, to prevent pressure on blood vessels and nerves.
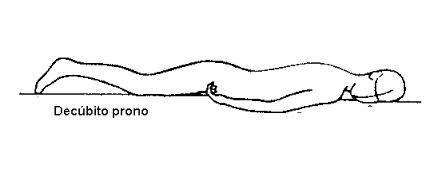
Prone, ventral or abdominal position
The person is lying on the chest and abdomen, with the head turned to one side, the upper limbs extended next to the body or flexed at the elbow, and the lower limbs extended.
Nursing Considerations:
This position may hinder lung expansion.
The person does not usually last long in a prone position, which must be taken into account when they are unable to turn around on their own.
Lateral decubitus
The person is lying on their side, with one side or the other on the surface, the upper limb on the side on which they are lying in front of the body, and the lower limbs extended, slightly flexed or with the one on top somewhat flexed and advanced. The name of lateral decubitus depends on the side of the body that is in contact with the horizontal plane: left or right.
Nursing considerations:
If the person has to remain in the lateral decubitus position for a long time, it is advisable to place a pillow between the legs to avoid compression of nerves and blood vessels.
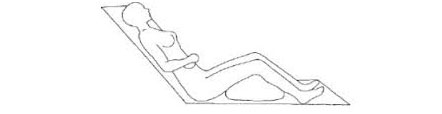
Fowler’s position
It is a dorsal position on an inclined plane in such a way that the back forms an angle of about 45 degrees with the horizontal. It is obtained by raising the head of the bed about 40-50 cm. The lower extremities can be kept flexed at a greater or lesser angle or kept extended. Sometimes we speak of a low (semi-Fowler) or elevated Fowler position, depending on the angle adopted by the back.
Nursing Considerations:
It is used to practice numerous techniques.
Provides greater comfort to people who have heart or respiratory problems.
Promotes drainage after abdominal operations.
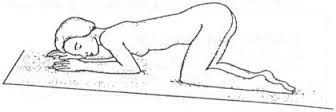
Genupectoral position
The person is placed on the bottom, supporting themselves on their knees and chest, with their head tilted and their thighs perpendicular to the bed.
Nursing Considerations:
This position is used to perform rectal examinations and procedures.
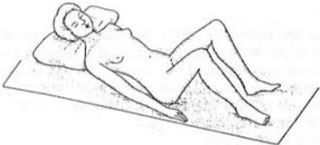
Gynecological or lithotomy position
It is a supine position with the legs bent over the thighs and the thighs abducted and flexed over the pelvis. It can be done on a special stretcher that has devices to keep the legs elevated, supporting the calves or feet on supports or stirrups.
Nursing Considerations:
This position is used for gynecological examinations, deliveries, rectal surgery, etc.
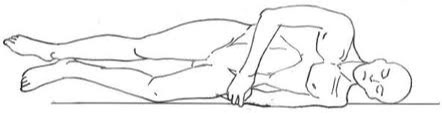
Rose or Proetz position
It is a supine position with the head hanging off the stretcher or operating table.
Nursing Considerations:
This position is used to prevent aspiration of blood or secretions, as well as in respiratory tract operations.
It is used to wash hair when the person cannot get out of bed.
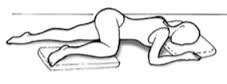
Sims position
It is a left lateral decubitus position with the arm and leg on this side extended and the right lower extremity flexed at the hip and knee. The left arm can be placed under the head or kept extended next to the trunk, so that the weight of the body rests on the chest.
Nursing considerations:
Used for vaginal and rectal examinations (manual and endoscopic), and to give enemas.
It is recommended as a safety position in the event of an accident with loss of consciousness and risk of vomiting.
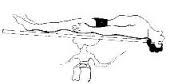
Trendelenburg position
It is a supine position on an inclined plane in such a way that the pelvis is higher than the head and the thighs are higher than the pelvis.
Nursing considerations:
It is used in surgery to perform operations on the lower abdomen and pelvis, and in some interventions on the lower limbs. The person is placed on a table inclined at 45 degrees, with the head down and the legs hanging, supported on an adjustable sector.
Inverted Trendelenburg position
It is the opposite position to the previous one, that is, with the person supine on an inclined plane in such a way that the head is higher than the feet.
Nursing considerations:
This position is used in surgery for interventions on the neck, face and skull, in order to reduce blood flow and prevent blood stagnation in the surgical area.
It is used in abdominal interventions to modify the situation of the viscera and better expose the operating field.